by Debra Cobb

From community masks and health workers’ kits, to hospital gowns, drapes and wraps, disposable personal protective equipment (PPE) is playing a critical role in the battle against COVID-19 infections. But now there is a mountain of disposable PPE that’s creating a whole new set of problems. Used masks and gloves are littering parking lots, city streets, country walks and showing up in our oceans and waterways. Hospital gowns, drapes and wraps—some uncontaminated—are being incinerated or dumped into landfills.
Practice Greenhealth, a Reston, Va.-based nonprofit health-care membership association that provides sustainability solutions, points out that hospitals produce an average of 30 pounds of waste per patient per day. According to its website, “Most hospitals are experiencing an increase in waste during the COVID-19 pandemic, primarily due to the increased use of disposable PPE.” As the pandemic continues, hospitals and other stakeholders are seeking more environmentally friendly PPE options that are cleanable, reusable or recyclable.
The case for reusable PPE
Most hospitals in the U.S. cite safety, cost and convenience as key reasons for choosing to use disposable nonwovens. Single-use, nonwoven polypropylene PPE may appear less costly on a per item basis, but it relies on sourcing from China, which currently controls some 80 percent of PPE manufacturing. Factor in the costs of shipping, current U.S. tariffs, and incineration or waste disposal, and a false economy emerges.
According to the American Reusable Textile Association, instead of being thrown out after each patient encounter, reusable isolation gowns can be washed, sterilized and reused 75 to 100 times. Laundering processes are being updated, moving out of hospital sites to regional clean room services with more energy-efficient equipment, where wash protocol and steam sterilization remove contamination, including particulate matter.
In additional to their environmental impact, disposable gowns and drapes often get negative feedback from surgeons and surgical technologists for thermal comfort issues, tearing and size, according to Project Greenhealth. Nelson Bebo, vice president of sales, Burlington® Medical, a division of Elevate Textiles™, adds that a key advantage of reusable fabrics is that they provide greater assurance of being available when critical PPE is needed most.
Headquartered in Greensboro, N.C., Burlington manufactures its range of Maxima® and XALT™ barrier fabrics for health care using state-of-the-art polyester yarns, constructions and finishes according to the Association for the Advancement of Medical Instrumentation® (AAMI) certifications and EN13795 European standards.
The durability of Burlington’s medical fabrics allows the life of the garment to be extended past its original use. For example, a fabric certified for Level 2 protection through 75 launderings can be tested at the end of that time and still meet certification for Level 1 protection, extending its life cycle.
Burlington operates its own on-site, institutional-grade medical laundry, complete with steam sterilization equipment. Fabrics are evaluated for true-to-life performance and durability before leaving the manufacturing facility.
“Burlington is known for innovation and quality, and we are proud to be a trusted supplier to leading PPE manufacturers globally,” says Bebo. “We take protection and our responsibility to provide it very seriously, and never has that been more important than now.
“The scarcity of equipment due to the COVID-19 crisis has reinforced the importance of reusable PPE, and we are pleased to offer our expertise to support the industry and ramp up the production of our proven, established fabrics to meet the current critical need.”
The company has seen production of its reusable health-care fabrics increase a whopping 500 percent during the coronavirus pandemic.
Filtration masks and reusability
According to the Nonwovens Institute (NWI) at North Carolina State University (NC State), the technology used in almost all masks for filtration is a meltblown fabric that is electrostatically charged, boosting the filtration efficiency from about 30 to 35 percent to more than 95 percent. Most meltblown fabrics are made from polypropylene and are not particularly robust. They cannot be reused, laundered or re-sterilized without a potential loss of electrostatic charge and reduction of the ability of the filter to protect the wearer—driving shortages of usable masks along with piles of disposed equipment.
The NWI is partnering with NatureWorks LLC, maker of sustainably sourced Ingeo™ polylactic acids (PLA) and biopolymers, to develop alternative filters using a bicomponent fiber of Ingeo and polypropylene.
“We took the spunbond technology and created a new generation of unique filters that have excellent filtering capability without needing to be charged, meaning they can potentially be reused after cleaning with peroxide or an alcohol solution,” said Behnam Pourdeyhimi, executive director of NWI and associate dean for industry research and extension, Wilson College of Textiles, NC State.
In Taiwan, Far Eastern New Century (FENC) Corp. announced the development of a sub-nanometer bicomponent fiber of polyester with polyethylene or nylon to replace the electrostatically charged meltblown polypropylene layer currently in use. According to FENC, the product can be repeatedly washed and offers bacterial filtration “far better than that of general medical-grade masks.”
The Korea Advanced Institute of Science and Technology (KAIST) is also testing a reusable nanofiber mask developed by Professor Il-Doo Kim. An electrospinning process was used to manufacture orthogonal nanofibers by controlling their alignment. This structure can minimize delivering the pressure toward the air filter and maximize the filtration efficiency.
In addition, a KAIST research team reports that Professor Kim’s nanofiber filter was “proven to be water resistant with more than 94 percent filtering efficiency in 20 repeated bactericidal tests with ethanol. The nanofiber mask also showed no deformation in its nano-membrane structure despite the 20 hand washes.”
When you can’t reuse, recycle
When PPE is based on a single polymer, such as polypropylene, sustainable recycling is another option for keeping used items out of the waste stream. The Welsh company Thermal Compaction Group (TCG) has come up with an innovation called Sterimelt.
Currently in use by a handful of National Health Service (NHS) hospitals in the U.K., the Sterimelt technology employs thermal heater plates to re-engineer a wide range of uncontaminated polypropylene nonwoven disposables into polypropylene blocks that can be resold to the plastics industry.
Tim Hourahine, technical compliance manager at TCG, explains, “In the U.K. alone an average 2.5 kg [5.5 pounds] of additional waste is being created during the pandemic by nurses discarding PPE after treatment of every patient and care home visit, every day. Sterimelt will reduce the volume of tray wrap, drapes, etc. by approximately 90 percent.
“The blocks can be sold back into the plastic supply chain and have commercial value. The reduction in waste through thermal compaction reduces regular transport needs, which reduces carbon footprint, makes the wrap recovery process sustainable and creates a full circular economy event.”
According to Hourahine, contaminated masks and gowns could potentially be included in the recycling process, as the heat used to melt the polypropylene is far higher than that of regular autoclave temperature, leaving the resulting materials sanitized at the end of the process. However, non-polypropylene materials such as cuffs, waistbands, ties and noseguards that are currently used on nonwoven PPE apparel items would contaminate the system, so for now, masks and gowns cannot be included.
Building on its Sterimelt recycling solution for single-use disposable tray wrap plastics, TCG is about to begin trialing a prototype CurtainMelt process for single-use disposable polypropylene bed, ward and cubicle curtains, which are currently replacing the old, linen-type ward curtains used worldwide.
“Plastics are not the problem; the way the human race discards plastic remains the issue,” Hourahine maintains. “Capturing single-use plastic at the point it becomes waste gives us at TCG the huge advantage to recover the polypropylene as a resource and treat it as such, by reducing its volume and sending it back into the supply chain as a much-needed, valued commodity.”
Debra Cobb is a freelance writer with extensive experience in the textiles industry. She lives in North Carolina.
SIDEBAR: Recyclable durability
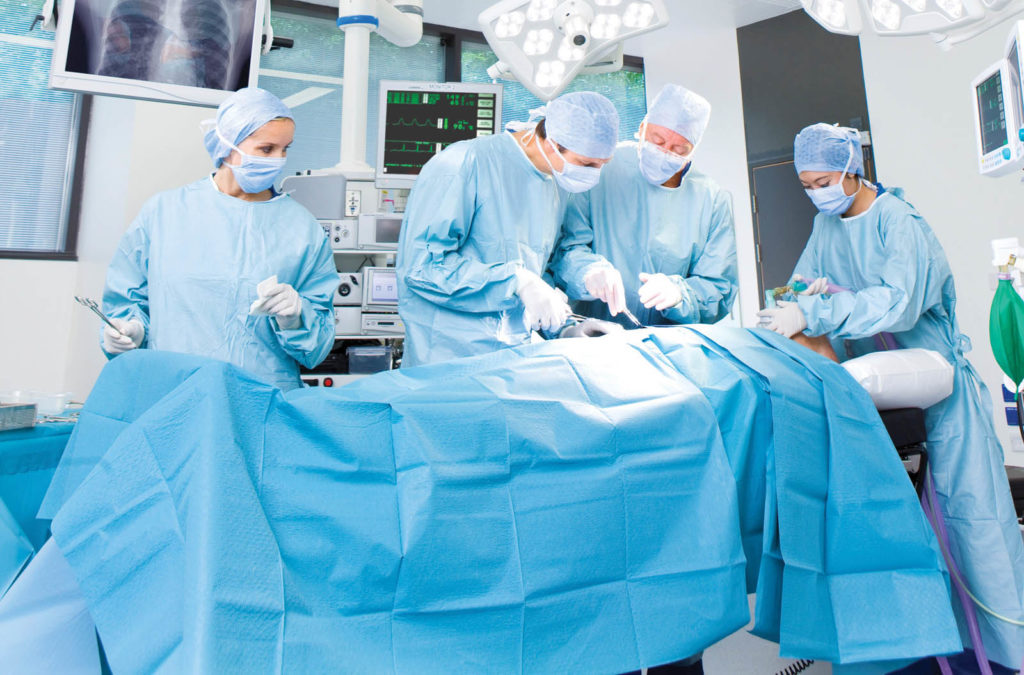
The durability of reusable barrier fabrics, such as those by Burlington® Medical, allow the life of a garment to be extended past its original use. According to the American Reusable Textile Association, instead of being thrown out after each patient encounter, reusable isolation gowns can be washed, sterilized and reused 75 to 100 times. Photo: Getty Images Cultura RF.
 TEXTILES.ORG
TEXTILES.ORG


